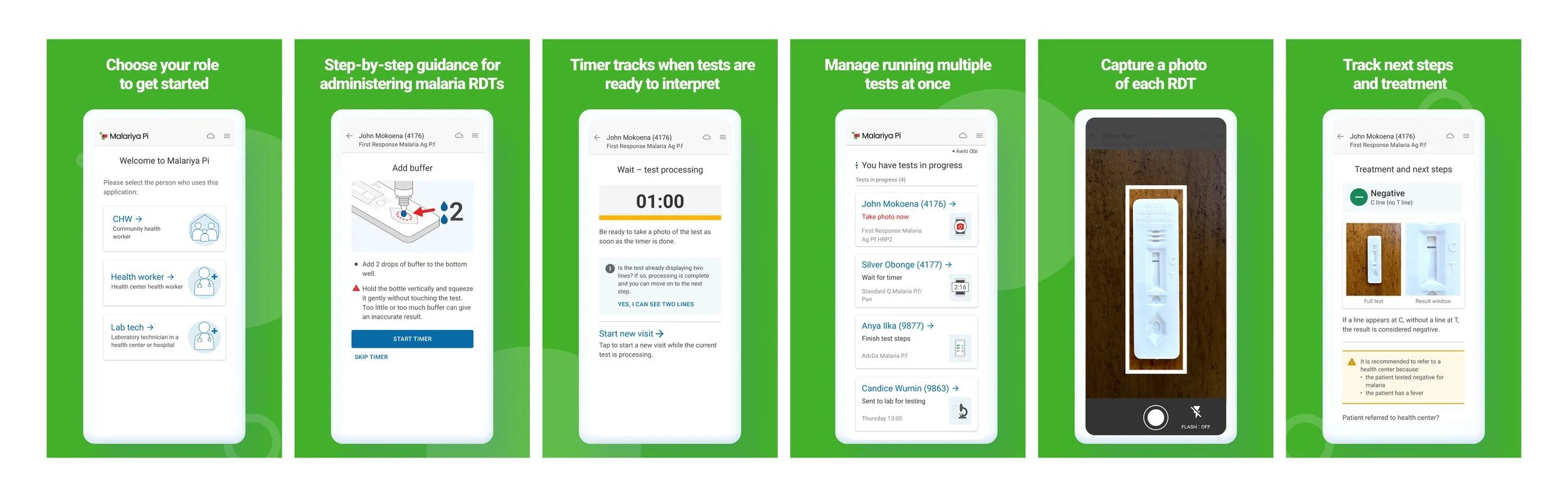
Malariya Pi — Digitizing Malaria Care in Rural Burundi
In Burundi, malaria incidence exceeds 500 cases per 1,000 people. Malariya Pi is an offline-first mobile solution designed to empower Community Health Workers (CHWs) and clinic staff. By integrating AI-powered Rapid Diagnostic Test (RDT) interpretation and an "offline cipher" referral system, we bridged the gap between remote villages and formal health centers.
Role: Lead UX Designer
Tools: Figma, Google Sheets/Docs
Context: Rural Burundi
Collaboration: Product, Engineering
Three distinct personas who interact with the same patient but have different environmental constraints:
Community Health Worker (CHW)
Primary Goal: Test and treat in the village; refer complex cases.
Pain Point: High isolation; no internet; limited clinical training.
Clinic Worker
Primary Goal: Manage high patient volume; intake or treat referrals.
Pain Point: Needs history of tests/meds administered in the field.
Lab Technician
Primary Goal: Administer specialized tests; provide result codes.
Pain Point: High speed; needs minimal data entry to maintain flow.
The referral code needed to be long enough to encode all of the necessary data, but not so long that it became tedious to write. 12 Characters was the balance needed.
The Problem: How to sync data with no internet?
The biggest UX hurdle was ensuring a Clinic Worker knew what a CHW did in the field without a database to pull from.
The Solution: The Offline Cipher.
We developed a system where the app generates a compressed referral code (cipher) based on intake details, test results, and drugs prescribed. This code is written on a paper transfer sheet. When the patient arrives at the clinic, the worker enters the code, and the app "unlocks" the patient’s history locally.
Design Decision: We prioritized a "paper-to-digital" hybrid workflow, recognizing that paper remains the most reliable fallback in low-power environments.